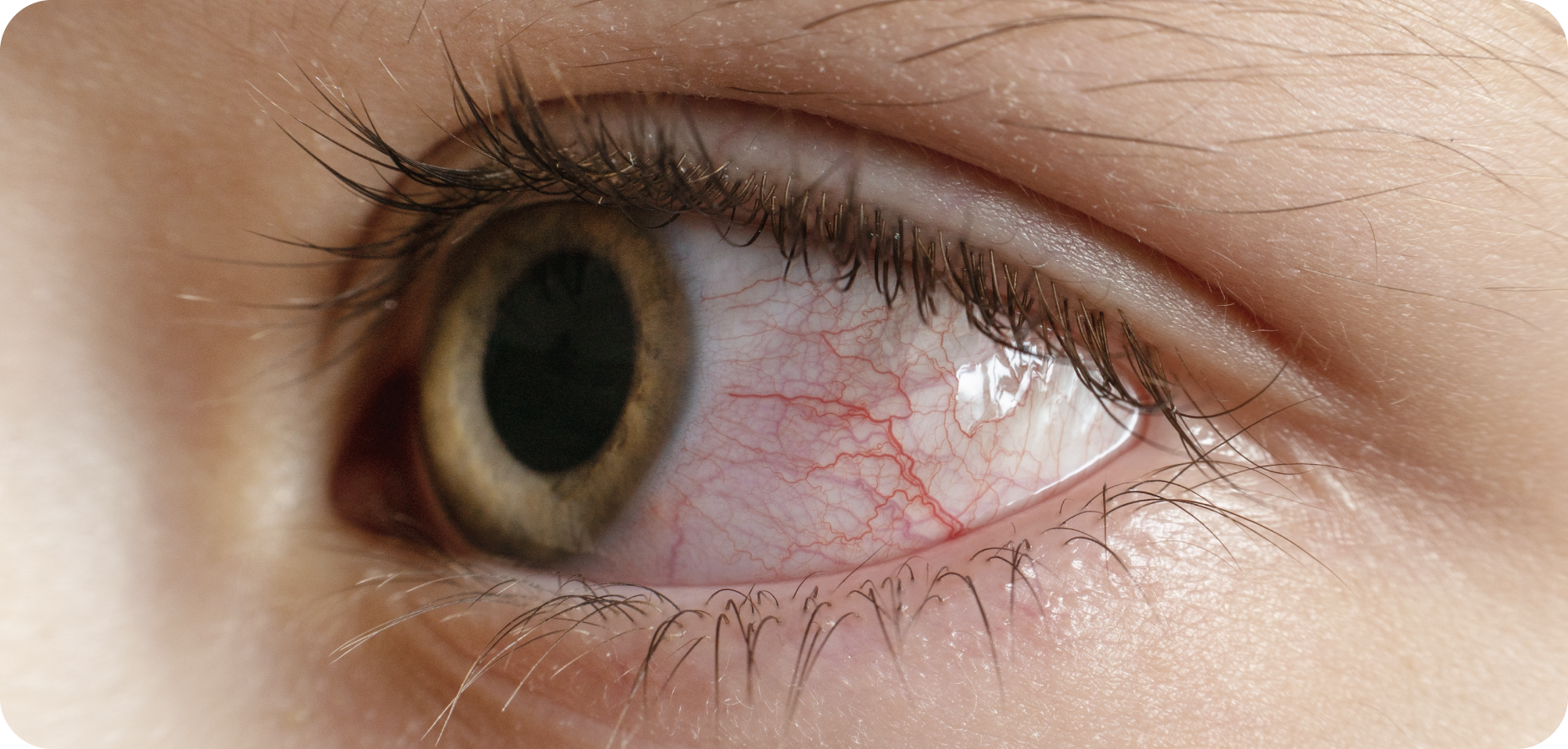
The cornea is the clear outer layer or shield covering the eye. While this shield usually protects the eye’s more delicate tissues, it can sometimes become damaged or infected.
For example, scratches may compromise the corneal surface and allow germs or bacteria to enter, leading to a cornea infection. Such infections can progress quickly and may even threaten vision.
A cornea infection refers to inflammation of the corneal tissue caused by microorganisms such as bacteria, viruses, fungi, or parasites.
The cornea has no blood vessels, making it more susceptible to rapid progression when infected. Even small injuries or surface defects can allow pathogens to enter and multiply.
Untreated or severe infections may lead to scarring, thinning, or perforation of the cornea. To minimise the damage, prompt treatment is advised.
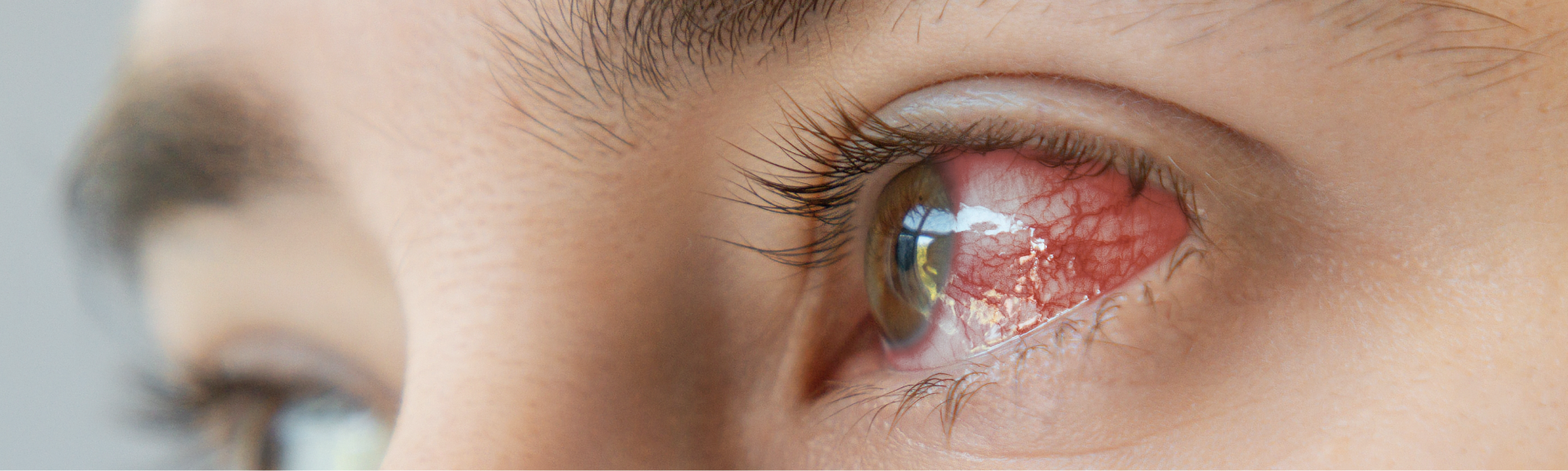
This is an eye infection that tends to be most common in contact lens wearers. It is caused by pathogens such as Staphylococcus aureus, Pseudomonas aeruginosa, and Streptococcus pneumoniae.
Bacterial keratitis progresses rapidly, to the point where corneal ulcers may develop within hours of its commencement. This makes treating it quickly a priority for patients.
The condition is strongly associated with the use of extended-wear lenses, poor lens hygiene, contaminated cases, and swimming or showering with lenses.
This is most frequently caused by Herpes Simplex Virus (HSV). Some of its symptoms are light sensitivity, tearing, discomfort, and dendritic epithelial patterns seen with fluorescein staining.
It can progress to stromal keratitis, which affects deeper layers and may lead to long-term scarring.
This is more common in tropical climates such as Singapore. It is caused by filamentous fungi (e.g. Fusarium, Aspergillus) or yeast (Candida).
The condition is typically seen after prolonged topical steroid use, or in patients with ocular surface disease. The fungus involved can be slow-growing but difficult to treat, and requires prolonged therapy in many cases.
This is a rare but severe parasitic infection caused by a free-living amoeba found in water and soil. It is most commonly linked to poor contact lens hygiene, rinsing lenses with tap water, or exposure to contaminated water while wearing lenses.
Treatment requires specific anti-amoebic medications and can be lengthy.
This condition is not caused by microbes but mimics early infection. The common triggers for it are severe dry eye disease, UV exposure from welding/sunlight, chemical irritation, or autoimmune conditions.
It is important to differentiate it properly from infectious keratitis because its management differs from the infectious version.
A cornea infection develops when the natural protective barrier of the eye is disrupted. Several habits, practices, or even conditions may be risk factors for that.

Many of the common guidelines for wearing contact lenses can help lower the risk of developing corneal infection. This means that the usual prohibitions for lens users apply.
As such, these can increase your chances of getting a cornea infection:
Chronic blepharitis or meibomian gland dysfunction often increases bacterial load near the cornea.
Meanwhile, severe dry eye disease predisposes a patient to epithelial breakdown, i.e. it makes the outermost layer of the cornea more likely to fail.
Foreign bodies, scratches from fingernails or makeup applicators, and plant matter injuries may allow organisms direct entry into the eye.
Humid climates favour fungal growth, so being in an environment like Singapore while lingering in areas with higher microbial exposure can make you more likely to get a fungal infection.
Systemic, chronic, and immune system conditions can make you more likely to develop the infection. Among other things, they weaken your immune system’s response to bacteria.
Autoimmune disorders can even affect the tear film, and as noted earlier, dry eye can make the cornea’s outermost layer more likely to break down.
Steroid drops may mask early symptoms of corneal infection and may even worsen or reactivate viral keratitis in particular. There is also a chance of them promoting fungal proliferation.

Corneal infections can present with a spectrum of symptoms.
Intensity varies by case, but generally, symptoms that worsen within hours warrant an urgent eye examination. The same is true if your symptoms persist for more than 24 hours.
If any of the following happen, you should consult an eye specialist immediately:
Early evaluation helps prevent structural complications, as the cornea heals less predictably than other tissues. Quick action is often the best way to improve outcomes for treatment.
Note that you should also avoid self-medicating with leftover eye drops, especially steroid drops. These have a chance of worsening some infections.
If a corneal infection is not treated quickly, certain complications (some of them permanent) may develop:
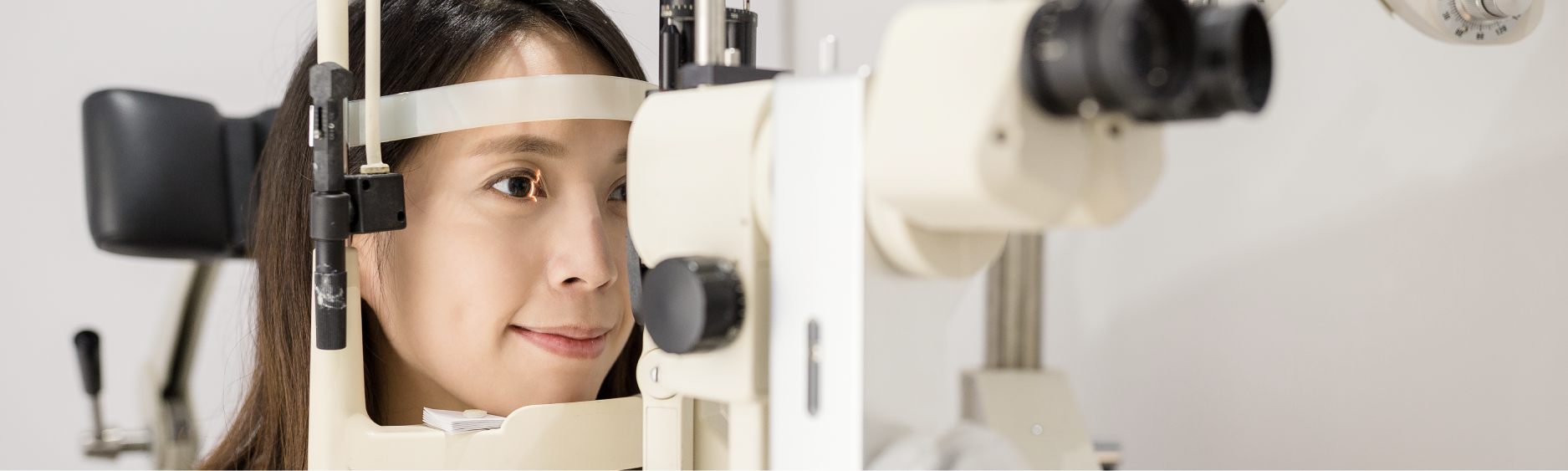
An ophthalmologist may perform several tests to check if you have a corneal infection, including these:
The specific treatment for corneal infection depends on the type of infection involved. Below are some of the more common approaches for the different types:
The treatment and healing time for cornea infections varies based on the cause and severity of the infection. Your doctor will generally schedule several follow-ups to monitor progress and treatment results.
Note that vision may also remain blurred during recovery in some cases, even after infection control.

You cannot guarantee that you will never get a cornea infection. However, here are some tips that reduce your risk:
A cornea infection is a potentially serious condition requiring prompt evaluation and appropriate treatment. If you believe you have the symptoms of such an infection, seek professional medical advice.
ERS Suntec City provides a comprehensive evaluation for corneal conditions. Book a consultation with ERS Suntec City’s ophthalmologists today and remember that early examination and care can often improve outcomes.